Hospital & Clinical Pharmacy - 1. Hospital Pharmacy
Hospital Pharmacy
In the past, the hospital has been a place for care of the sick. Today the hospital has become a center of technical services for the sick and well, in patients as well as outpatients, with greater emphasis on achieving the highest standard of patient care and community health.
Definition of Hospital:
A hospital is a healthcare institution with an organized medical and professional staff, equipped with permanent facilities including inpatient beds that provides medical, nursing, and other health-related services to patients.
Definition of Hospital Pharmacy:
A hospital pharmacy is a department within a hospital that manages the procurement, storage, compounding, and dispensing of medications. It also provides clinical services, such as medication therapy management, patient counseling, and drug information, to ensure safe and effective medication use for inpatient and outpatient care.
Scope of Hospital Pharmacy
- Dispensing: Ensure accurate, safe medication delivery, checking for allergies and interactions.
- Management: Collaborate on therapy plans, review prescriptions, monitor patient response.
- Safety: Prevent errors, conduct reviews, educate on safe use, minimize adverse events.
- Clinical Services: Provide direct care, reconcile meds, advise teams and patients.
- Preparation: Compound specialized or sterile meds as needed.
- Formulary: Manage approved drug list based on safety, efficacy, and cost.
- Research: Lead trials, evaluate medication use, and drive improvements.
- Goal: Ensure safe, effective medication use through team-based patient care.
- Regulatory Compliance: Hospital pharmacists ensure that the pharmacy operations adhere to local, state, and federal regulations regarding medication handling, storage, and dispensing.
- Collaboration with Healthcare Team: Pharmacists work closely with physicians, nurses, and other healthcare professionals to provide comprehensive patient care and participate in interdisciplinary healthcare teams.
Organizational Structure of a Hospital Pharmacy
The organizational structure of a hospital pharmacy can vary depending on the size of the hospital, the number of patients it serves, and its specific needs. However, in general, a hospital pharmacy typically follows a hierarchical structure with the following key roles:
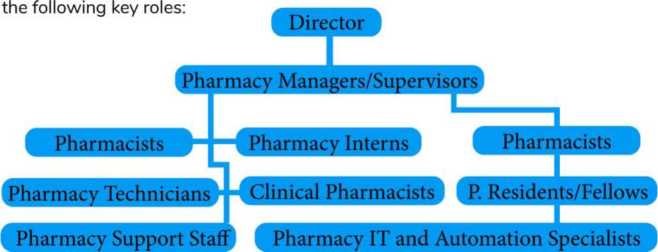
- Director of Pharmacy: At the top of the hierarchy is the Director of Pharmacy, who oversees all pharmacy operations and is responsible for developing policies, setting goals, and managing the pharmacy budget.
- Pharmacy Managers/Supervisors: Reporting to the Director of Pharmacy, there are one or more Pharmacy Managers or Supervisors. They are responsible for managing the daily operations of different pharmacy departments or units, such as inpatient pharmacy, outpatient pharmacy, sterile compounding, or clinical services.
- Pharmacists: Pharmacists are licensed healthcare professionals who play a crucial role in the hospital pharmacy. They work closely with healthcare teams to ensure proper medication management, dosage, and administration. Pharmacists may specialize in various areas, such as clinical pharmacy, oncology pharmacy, or infectious disease pharmacy.
- Pharmacy Technicians: Pharmacy Technicians work under the supervision of pharmacists and assist in various pharmacy tasks, including medication dispensing, inventory management, and administrative duties.
- Pharmacy Interns: Some hospital pharmacies employ pharmacy interns who are still in the process of completing their education and licensure requirements. They work under the guidance of pharmacists and gain practical experience.
- Clinical Pharmacists: Larger hospitals may have clinical pharmacists who are involved in patient care rounds, collaborating with healthcare teams to provide medication therapy management and ensuring safe and effective drug use.
- Pharmacy Residents/Fellows: Pharmacy Residents and Fellows are highly trained pharmacists who have completed their Doctor of Pharmacy (PharmD) degree. These positions are designed to provide advanced training and specialization in various areas of pharmacy practice, enabling pharmacists to become experts in specific fields.
- Pharmacy Support Staff: In addition to pharmacy technicians, there may be other support staff, such as pharmacy aides or administrative personnel, who assist with non-clinical tasks.
- Pharmacy IT and Automation Specialists: As technology plays an increasingly vital role in modern pharmacy operations, some hospitals may have specialists who manage pharmacy information systems and automation equipment.
Qualifications and Experience requirements for Hospital Pharmacists
The qualifications and experience requirements for hospital pharmacists can vary depending on the country and healthcare system. However, in general, the following qualifications and experiences are typically required to become a hospital pharmacist:
Educational Qualifications:
- D. Pharm (Diploma in Pharmacy): 2-year course; eligible for hospital pharmacist posts.
- B. Pharm (Bachelor of Pharmacy): 4-year degree; preferred for advanced roles.
- PharmD (Doctor of Pharmacy): 6-year professional doctorate; includes advanced clinical training (less common, but increasingly recognized).
Registration:
Must register with the State Pharmacy Council under the Pharmacy Act, 1948, after completing the required qualification.
Practical Experience:
Internship/training during coursework is mandatory (especially in PharmD and B.Pharm). Hospital roles may prefer candidates with prior hospital or clinical training.
Skills and Competencies:
- Clinical Knowledge: Clinical knowledge of drugs, interactions, and guidelines.
- Communication Skills: Strong communication skills with healthcare teams and patients.
- Analytical Skills: Analytical skills for reviewing medication orders and ensuring patient safety.
- Technological Proficiency: Basic proficiency in hospital pharmacy software/EHR.
- Regulatory Knowledge: Awareness of Pharmacy Act, drug regulations, and hospital protocols.
Continuing Education:
Required to maintain registration and stay updated with advances in pharmacy practice.
Additional Certifications (Optional but Beneficial):
- Certified Geriatric Pharmacist (CGP)
- Certified Diabetes Educator (CDE)
- Advanced Cardiac Life Support (ACLS)
- Basic Life Support (BLS)
Requirement of the Pharmacist as per the bed requirement
| Bed strength | Number of Pharmacist required |
|---|---|
| Upto 50 beds | 3 pharmacist |
| Upto 100 beds | 5 pharmacist |
| Upto 200 beds | 8 pharmacist |
| Upto 300 beds | 10 pharmacist |
| Upto 500 beds | 15 pharmacist |
Inter-professional relationships
Hospital pharmacists maintain professional relationships with various individuals and groups within the healthcare setting. These relationships are essential for providing quality patient care, promoting medication safety, and ensuring effective communication and collaboration among healthcare professionals. Some of the key professional relationships of a hospital pharmacist include:
- Physicians: Hospital pharmacists work closely with physicians to review medication orders, suggest appropriate drug therapy, and provide drug information. They collaborate on treatment plans and discuss potential drug interactions or adverse effects to ensure patient safety and optimal outcomes.
- Nurses: Pharmacists interact with nurses regularly, especially during medication administration. They may clarify medication orders, address nursing concerns, and provide education on proper drug administration techniques.
- Patients and Their Families: Pharmacists develop relationships with patients and their families to provide counseling on medications, answer questions, and ensure medication adherence. Building trust and rapport with patients can help improve medication compliance and overall patient satisfaction.
- Pharmacy Technicians: Hospital pharmacists work closely with pharmacy technicians to ensure the accurate and timely preparation and dispensing of medications. They provide guidance, supervision, and support to pharmacy technicians to maintain a smooth workflow in the pharmacy.
- Other Allied Health Professionals: Hospital pharmacists collaborate with various allied health professionals, such as dietitians, respiratory therapists, physical therapists, and occupational therapists. They exchange information and coordinate care to optimize patient outcomes.
- Pharmacy Students and Residents: Hospital pharmacists often serve as preceptors for pharmacy students and residents. They provide mentorship, supervise training activities, and help develop the next generation of pharmacists.
- Pharmacy and Therapeutics (P&T) Committee: Hospital pharmacists participate in P&T committees, which are responsible for evaluating medications, formularies, and making decisions about drug use within the hospital. They contribute their expertise to ensure evidence-based and cost-effective medication choices.
- Quality and Safety Teams: Pharmacists actively participate in quality improvement initiatives and patient safety programs within the hospital. They contribute their knowledge and experience to enhance medication-related processes and reduce medication errors.
- Health Information Technology (IT) Team: Hospital pharmacists work with the IT department to ensure proper functioning of medication management systems, electronic health records, and other technology related to pharmacy operations.
- External Pharmacy Organizations: Pharmacists often engage with local, state, and national pharmacy organizations. These associations provide opportunities for professional development, networking, and staying updated on the latest advancements in pharmacy practice.
Good Pharmacy Practice (GPP) in a hospital (Model Answer)
Definition:
Good Pharmacy Practice (GPP) defines pharmacists as providing quality pharmacy service to every patient. It is the practice of pharmacy that responds to the needs of the people, who use the pharmacists’ services to provide optimal, evidence-based care.
Following are the important requirements of good pharmacy practice:
- A pharmacist’s first priority must be the welfare of the patient.
- A pharmacy service must supply medication and health care products of assured quality and must monitor the effects of their use.
- A pharmacy service must contribute in the promotion of rational and economical prescription and appropriate use of medicines.
- Each element of pharmacy services must be relevant, clearly defined, and effectively communicated to all involved.
- It requires to convert all activities in a smooth manner with zero defect level.
- Pharmacist gives appropriate information and advice about use of medicine.
- Pharmacists promote prescribing and dispensing methods that are rational and economical.
- Pharmacists work together with other health care professionals for improving patient safety.
FIP Basel Statements (Model Answer)
Introduction:
- FIP (International Pharmaceutical Federation) is a global federation of national associations of pharmacists and pharmaceutical scientists.
- In 2008, hospital pharmacists all over the world met in Basel, Switzerland to discuss the future of hospital pharmacy, hosted by FIP.
- In 2014, they again gathered in Bangkok and launched the updated version of the Basel statement with 65 statements. These statements cover the following six main areas of hospital pharmacy.
Six Main Areas of Basel Statements:
- Procurement
- Influence on prescribing
- Preparation and delivery of medication
- Medication administration
- Monitoring Medication
- Human resources, training & development
1. Procurement:
- Ensures that medications are obtained from reliable sources to maintain quality, safety, and cost-effectiveness.
- Involves selecting, purchasing, and securing medicines that meet patient and institutional requirements.
2. Influence on prescribing
- Engages pharmacists and healthcare teams to guide the choice of medications based on best practices and formularies.
- Promotes evidence-based, rational prescribing to enhance patient outcomes.
3. Preparation and delivery of medication
- Focuses on accurately compounding, packaging, and labeling medicines to ensure correct dosing and minimize errors.
- Ensures timely and secure distribution of medication to patients or wards.
4. Medication Administration:
- Oversees the process of giving medicines to patients, ensuring the right dose reaches the right patient at the right time.
- Aims to uphold safety and adherence to prescribed therapy.
5. Monitoring Medication:
- Involves continuous assessment of patient response and detection of adverse effects or interactions.
- Supports adjusting therapy as needed for safety and efficacy.
6. Human Resources, Training & Development:
- Ensures pharmacy staff are well-trained and updated on latest pharmacy practices and regulations.
- Invests in professional development to maintain competency and improve healthcare quality.
American Society of Health-System Pharmacists (ASHP)
Introduction:
- The American Society of Health-System Pharmacists (ASHP) is the largest professional organization in the United States dedicated to supporting pharmacists who practice in hospitals, health systems, ambulatory care clinics, and other organized healthcare settings.
- Founded in 1942, ASHP represents over 60,000 members including pharmacists, pharmacy technicians, and pharmacy students, advocating for optimal, safe, and effective medication use across healthcare environments.
Mission and Contributions:
- ASHP’s mission is to help its members achieve the best health outcomes for patients by advancing pharmacy practice through education, professional development, and establishment of evidence-based standards.
- The organization is known for developing influential policy positions, offering comprehensive resources, and serving as the accrediting body for pharmacy residency and technician training programs in the United States.
- ASHP also publishes leading references such as the AHFS Drug Information Book and the American Journal of Health-System Pharmacy.
Advocacy and Impact:
- ASHP is involved in advocacy, representing the interests of pharmacists in policy discussions with regulatory bodies like the FDA and CDC on medication use and public health issues.
- The society plays a key role in ensuring high standards of care, promoting patient safety initiatives, maintaining a national database on drug shortages, and driving continuous quality improvement in pharmacy practice nationwide.
Introduction to NAQS Guidelines
Introduction:
- The National Quality Assurance Standards (NAQS) are a set of benchmarks designed to ensure the delivery of high-quality healthcare services in public health facilities across India.
- Developed by the Ministry of Health & Family Welfare, these standards are intended for use in various healthcare settings, including district hospitals, community health centers, and primary health centers.
- NAQS guidelines offer a structured, evidence-based framework to promote patient safety, effective service delivery, and continuous quality improvement.
Eight Main Areas of NAQS Standards:
- Service provision
- Patient rights
- Inputs (resources)
- Support services
- Clinical care
- Infection prevention and control
- Quality management
- Outcome measurement
Key Focus Areas:
- Patient-centered care and respect for patient rights
- Proper infrastructure and equipment management
- Safe medication practices and infection control
- Regular staff training and development
- Robust documentation and feedback systems
- By adhering to NAQS, healthcare facilities can ensure regulatory compliance, minimize lapses in care, foster accountability, and enhance patient satisfaction.
- The guidelines support a culture of quality and transparency, laying the foundation for accreditation and nationwide improvement in health outcomes.
NABH Accreditation
Introduction:
- NABH Accreditation is a quality certification granted to healthcare organizations in India by the National Accreditation Board for Hospitals & Healthcare Providers (NABH), a part of the Quality Council of India.
- Established in 2006, NABH’s mission is to set rigorous benchmarks for quality and patient safety, ensuring that accredited hospitals and clinics adhere to globally accepted standards of healthcare delivery.
Accreditation Process:
- The process assesses a healthcare facility on a wide array of parameters spanning patient-centered areas—such as patient rights, access, and continuity of care.
- Also includes organization-centered areas like infection control, infrastructure, information management, and operational protocols.
- Hospitals must meet hundreds of objective criteria across ten chapters to qualify.
Benefits of NABH Accreditation:
- Signals that the facility maintains high standards, enhancing credibility, operational efficiency, and trust.
- Aligns Indian hospitals with international healthcare standards and is recognized by the International Society for Quality in Health Care (ISQUA).
- Supports medical tourism and global recognition.
- Fosters ongoing quality improvement, patient safety, and institutional accountability within India’s healthcare system.
Role of Pharmacists
Key Responsibilities:
- Involved in the procurement, storage, preparation, labeling, and distribution of medications.
- Review prescriptions for accuracy, advise on drug selection, dosage, and administration, and monitor for adverse drug reactions or interactions.
- Participate in patient counseling, provide drug information and education, and conduct clinical audits to promote rational pharmacotherapy and adherence to guidelines.
- Ensure compliance with regulatory standards, manage controlled substances, and contribute to continuous quality improvement in patient care processes.